AI Workforce for Revenue Growth: Autonomous RCM from Note to Claim.
A real-time validation engine designed to ensure every clinical note translates into a fully reimbursable claim, eliminating the friction between care delivery and financial recovery.
Unified Intelligence Architecture
We consolidate three critical functions into a single autonomous workflow, creating a frictionless path from encounter to payment.
AI Medical Coder
Advanced NLP translates nuanced clinical intent into precise ICD-10 and CPT codes without human intervention.
AI Denial Predictor
Scans every claim against proprietary payer-specific logic to flag issues before they ever leave your clearinghouse.
AI Revenue Recovery
The final layer of defense, automating the identification and recovery of underpaid or wrongly denied accounts.
Real-Time Coding Alignment
Stop waiting for post-encounter reviews. AI Workforce for Revenue Growth extracts diagnoses and procedures directly from clinical notes in real-time, highlighting potential gaps while the physician is still focused on the patient.
- check_circle Automatic CPT/ICD-10 suggestion engine
- check_circle Direct EHR integration via FHIR protocols
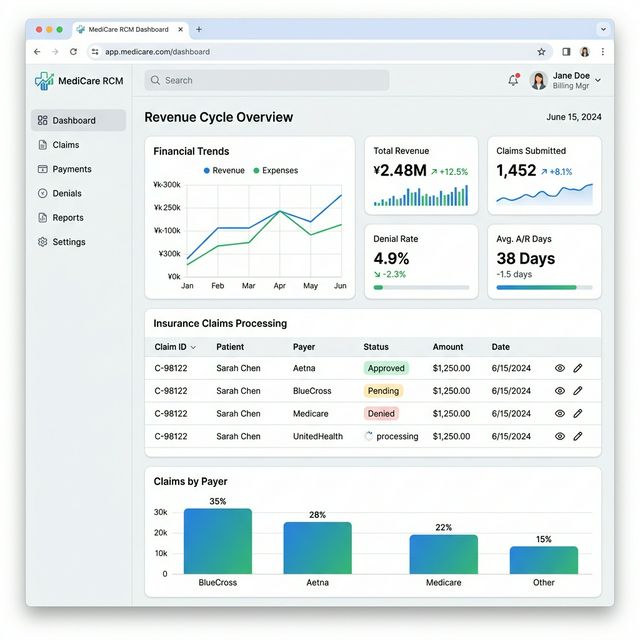
Real-Time Coding Alignment
Stop waiting for post-encounter reviews. AI Workforce for Revenue Growth extracts diagnoses and procedures directly from clinical notes in real-time, highlighting potential gaps while the physician is still focused on the patient.
"Missing modifier 25 based on payer policy update as of Jan 12th."
Unprecedented Operational Impact
By removing the manual heavy lifting of revenue cycle management, we empower your team to focus on high-value exceptions rather than routine processing.
Appeal Reduction
Reduction in time spent on manual appeal letter preparation and clinical evidence gathering.
First-Pass Acceptance
The industry benchmark for organizations utilizing our proactive denial prevention engine.
Financial Health Score
Ready to achieve Revenue Autonomy?
Join leading health systems utilizing AI Workforce for Revenue Growth to protect their margins and streamline provider workflows.